Relevance of the topic: Neuropathic pain is defined as "pain caused by primary damage to the nervous system or its disfunction". It occurs for a variety of reasons, and is mainly chronic and is usually not stopped by the use of conventional analgesics [1,2,3]. According to various estimates, the prevalence of this pathology is 50-115 cases per 100,000 population [4].
Neuropathic pain is formed against the background of persistent pain as a result of increasing overexcitation or damage to peripheral and/or central pain structures and is characterised by particularly severe pain and disorders of different types of sensitivity. Neuropathic pain is based on complex mechanisms: disruption of neuronal ion channels, overexcitation of neurons due to excessive intake of Ca2+ ions, prostaglandins; release of special pain neurotransmitters (glutamate, nitrogen oxide, neurokinin, prostanoids, etc.) in spinal pain structures. Neuropathic pain syndrome can be the result of cancer and non-oncological diseases, severe injuries and surgical interventions (phantom, post-torocotomic, postcholecystectomy, etc.). Neuropathic pain can develop from simple nociceptive pain syndrome due to its ineffective therapy [5].
Neuropathic pain is characterised by a combination of sensory positive and negative symptoms, which can be different, as well as change during the disease. It is the careful clinical analysis of sensory disorders that is the basis for diagnosing neuropathic pain [6].
This study aimed to study: the nature of neuropathic pain in patients with neurological disorders with the prospect of improving the diagnosis of neuropathic pain.
Materials and methods: Data was conducted in South Kazakhstan region with the help of a modified Pain DETECT questionnaire. In total, the questionnaire provides 12 questions to identify the intensity and nature of pain, prevalence, etc. The study involved 102 patients with neurological disorders and signs of neuropathic pain: 59 (57.8%) - men and 43 (42.2%) - women. Respondents are divided into age groups: up to 40 years (26 people or 25.5%), 41-50 years (25 people or 24.5%), 51-60 years (29 people or 28.4%) and 60 years and older (22 people or 21.6%). The collected material and results are preliminary (it is planned to increase the sample to 1000 respondents). The standard methodology calculated the relative indicator and average error. The Pearson Che Square method was used to study the statistical relationship.
Results and discussion: According to the results of the survey, it was established that in the main proportion of patients (81.3±3.86%) with neurological disorders, the intensity of the most severe pain attack over the past 4 weeks is 8-10 points on the measurement scale from 0 to 10 points ( figure 1).
Severe pain attack over the past 4 weeks is slightly higher than in the female population. However, there is no statistically reliable connection between the intensity of pain and the sex sign (χ2=3.94, df=4, p=0.42).
16
Unlike gender, age determines the intensity of pain in patients with neurological disorders (χ2=21.01, df=12, p=0.05). Less intense pain is stated by patients in the age group 51-60 years and groups older than 60 years, and more intense pain, respectively, in the age group up to 40 years and 41-50 years.
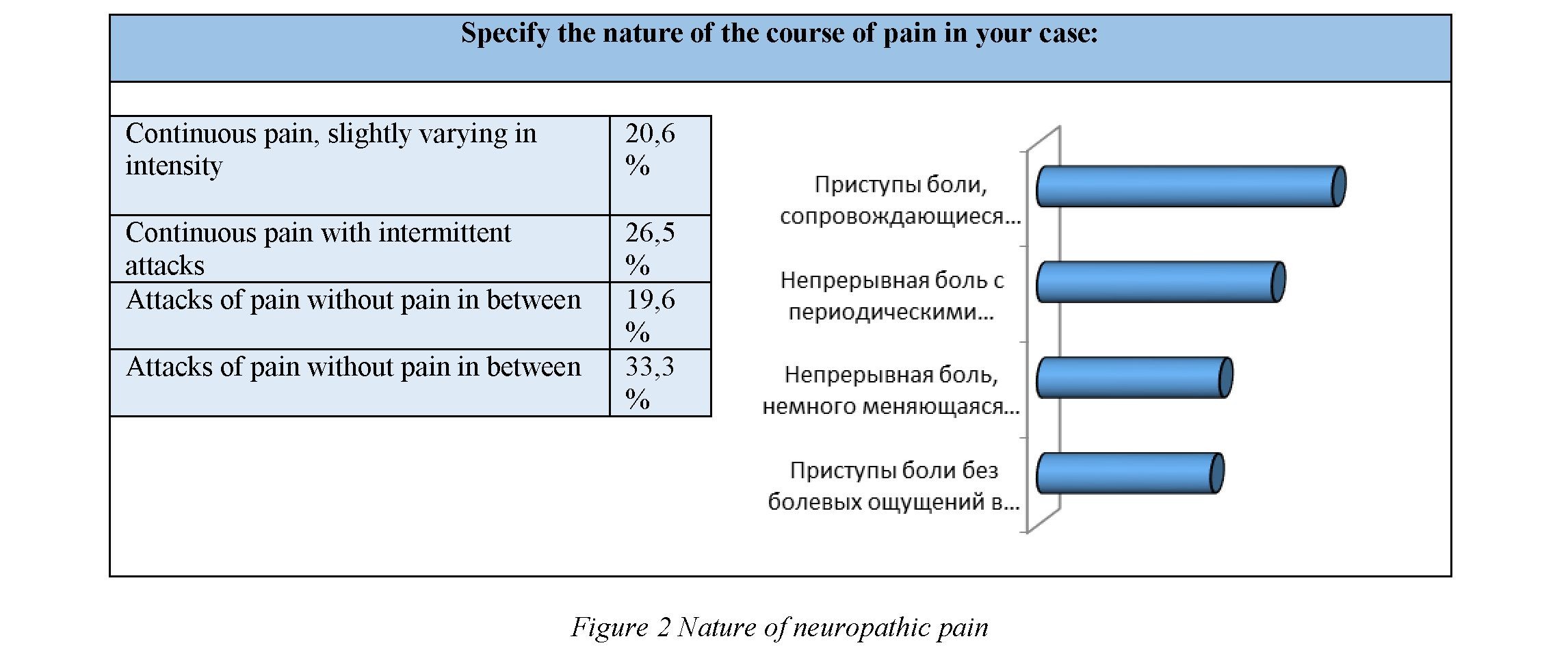
Characterising pain, 33.3±4.67% of patients noted that "pain attacks are accompanied by pain in between", 26.5±4.37% noted that "pain is continuous, with periodic attacks", 20.6±4.00% noted that "pain is continuous, slightly changing in intensity" and 19.6±3.93% noted that «painless pain attacks between neither» (figure 2).
Df=3, p=0.74), but is influenced by its age (χ2=15.85, df=9, p=0.05). Differences in the nature of pain on the sex are not significant. Age groups are characterised by the following: at the age of 40, patients are characterised by continuous pain (53.9±4.94%), at the age of 60 years and older patients are characterised by pain attacks (63.6±4.76%), and at the age of 41-60 patients equivalently (50/50) there are continuous pain and pain attacks.
According to the results of patients' answers (each answer in the questionnaire was assigned a certain coefficient), the total number of points was calculated, on the basis of which the final conclusion was made that there was a neuropathic component of pain: the negative result (3.9±1.92%) showed the unlikely that there was a neuropathic component of pain, the uncertain result (14.7±).
Conclusions: neuropathic pain in patients with neurological disorders is quite intense and is due to the age of patients;
The nature of neuropathic pain is ambiguous and depends on the age of the patient;
The intensity and nature of neuropathic pain in the male and female populations are equivalent.
The list of references:
- Danilov A. B., Davydov O. Village Neuropathic pain // Moscow: Borges. - 2007. - T. 2. - No. 007. - S. 6-10.
- Kamchatnov P. R. Neuropathic pain: possibility of pregabalin use // Consilium medicum. - 2007. - T. 9. - No. 2C. - S. 140-142.
- Markin S. P. Modern view of the problem of spinal pain // Russian Medical Journal. - 2009. - T. 17. - No. 11.
- Danilov A. B., Davydov O. Village Central neuropathic pain: clinical and diagnostic aspects and possibilities of therapy based on evidence // neurology. - 2009. - S. 60.
- Osipova N. A., Abuzarova G. R., Petrova V. C. Principles of analgesic use in acute and chronic pain // Moscow. - 2011- No. 4-5-C. 28-32.
- Turbina L. G., Gordeev S. A. Neuropathic pain: pathogenesis, clinic, diagnosis, treatment // Doctor. - No. 5-C. 56-60.
17