Platelet-rich plasma (PRP) is a blood product with a high platelet level that is widely applicable in different branches of medicine nowadays [1, 2]. The purpose of this study was to answer the question: “Would the application of PRP be effective in acute and postsurgical wounds healing?” based on the results of studies.
Material and methods: The literature search was conducted through MEDLINE, EBSCO, Cochrane Databasefor the termsPRP, Platelet Rich Plasma, Platelet therapy, Wound Healing, Acute wounds.Articles relating to the use of platelet rich plasma in surgery and wound healing after 2006 were included.
Results: Among 141 studies 37 were devoted to studies of the use of PRP in animals and 44 in humans. Controlled studies have shown a significant positive effect of PRP on the healing of acute and postoperative wounds. Nevertheless, two controlled studies did not show differences between two study groups.
Conclusion: In most studies, the effectiveness of PRP in acute and postoperative wounds healing was proven.The positive effect of PRP on the rate of epithelialization and the reduction of complications in the postoperative period was noted.
Introduction.
Autologous platelet-rich plasma (PRP) is a blood product that is widely applicable in different domains of medicine such as traumatology, sports medicine, general surgery, gynecology, dermatology, ophthalmology, dentistry and plastic surgery. Published studies indicate that administration of PRP directly into the wound or its application on the wound surface is recognized as successful choice of the treatment method in various cases of wounds'etiology [1-4]. It is evidenced that PRP plays an important role in physiological regeneration [5].
Despite the fact that a wide range of clinical studies confirm the considerable impact of PRP on wounds' healing, there are studies, showing absence or limited efficiencyof plasma treatment. Inconsistency of results about efficient usage of PRP shows necessity for further analyzes of collected data.
The usage of PRP represents in some cases the method of choice for setting off natural regeneration mechanisms owed to growth promoting substance in platelets [6]. PRP is a convenient and safe biological "tool", accelerating regenerative processes through launching all parts of the natural regeneration processes simultaneously and acting on them synergistically [7].
Purpose: To study the effectiveness of autologous platelet rich plasma usage on the healing of acute and postsurgical wounds with reference to the world literature.
Material and methods:
Search in databases: MEDLINE Complete, eBook Clinical Collection (EBSCOhost), Cochrane Central Register of Controlled Trials, Database of Abstracts of Reviews of Effects, Cochrane Database of Systematic Reviews, NHS Economic Evaluation Database, Health Technology Assessments, Cochrane Methodology Register are represented by two scholars and the main author-consultant.
Inclusion criteria:uncontrolled and controlled studies (randomized, prospective, retrospective with evaluation of the results of the usage of platelet-rich plasma in the treatment of wounds);full text scientific articlein English language; articles published after 2006; controlled trials with platelet-rich plasma application in the primary group and no treatment or treatment with standard method in the control group;articles presenting studies on rich plasma application in acute wound healing process.
Exclusion criteria: abstracts, repeating articles; articles published before 2006; non-English articles; case reports;review articles;combination of PRP-therapy with other treatment methods in the primary group; articles reporting in vitro studies. The process of selection of data and their analysis comprises a number of steps following an algorithm focused on three major referent points: the type of wounds, the treatment method applied and the clinical outcome (Figure 1).
Figure 1 - Flow chart

Results and discussion:
The search started by using keywords. The total number of relevant titles was 940, including 208 full-text original articles, which had been finally selected for the analysis. Hereafter among the selected articles in English from the period after 2006 only 141 works had been chosen. Among them 27 were presenting in vitro research, 37 studies on animals and 44 clinical trials on humans. In addition there were 9 case report studies and 24 review articles (Figure 2).
■ clinical studies on humans
31%
■ studies on animals
■ in vitro
■ review articles
19%
■ case-studies
26%
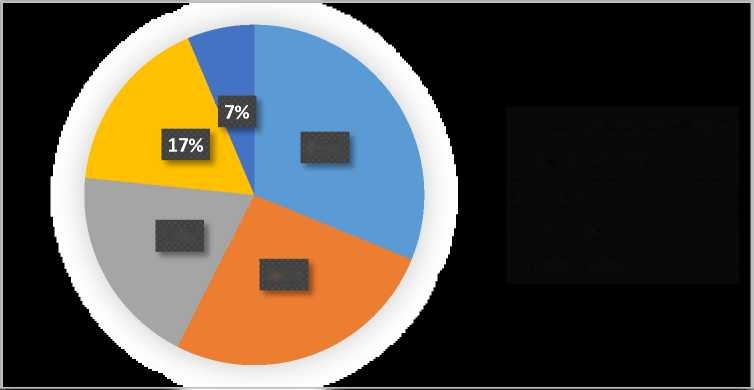
Figure 2 - The structure of scientific research of platelet-rich plasma
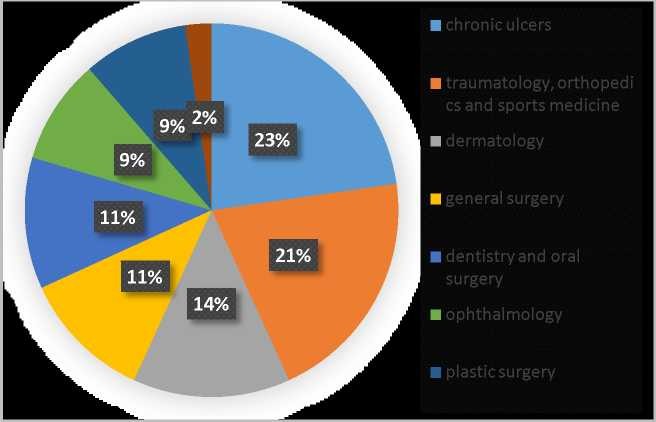
44 clinical trials on humans consisted of 22 uncontrolled and 22 controlled trials. As the purpose of this study was to answer the question: “Would the application of PRP be effective in acute and postsurgical wounds healing?”We determined the field of medicine in all presented clinical trials, which describe use of PRP. Thus, 10 works have been devoted to the study of the usage of PRP in the treatment of chronic ulcers of the lower extremities
- vascular and neurotrophic, 9 works examined the usage of platelet-rich plasma in traumatology, orthopedics and sports medicine, 6 - in the field of dermatology, 4 - in the field of ophthalmology, 5 - in general surgery, including thoracic and proctology, 5 - in dentistry and oral surgery, 4 - plastic surgery, 1
- in cardiac surgery (Figure 3).
Figure 3 - The field of medicine, where the results of the study of the efficacy of platelet-rich plasma are presented
We were interested in studies held on animals and humans. Preference was given to those works which purpose was to determine the efficacy of platelet-rich plasma in the healing of various acute and postsurgical wounds. Despite the fact that controlled studies obtain the greater reliability, we have also separately considered uncontrolled studies held on humans. Several studies - Han. (2007), Molina-Minano (2009), Ostvar (2015), Cho-HeeJee (2016), Hom (2007), Kazakos (2008), Spyridakis (2009), Kakudo (2011),Iervolino (2013), Prochazka (2014) give statistically-significant evidences that the use of PRP leads to the acceleration of wounds healing and other positive effects [8 - 17]. Three controlled studies held by Lee (2008),Khalafi (2008), Danielsen (2008) have not revealed any differences in the speed of wound healing [18 - 20] and level of pain in early postoperative period [21]. One of the studies, focused on the quality of life and the measurement of pain during the postoperative period also stated the absence of differences between the results in two groups [22]. Nevertheless, the application of histological techniques confirmed the acceleration of wound healing process in experimental animal studies [9 - 11](see Table 1).
However, most of publications showed positive results of the platelet-rich plasma application, affecting the rate of healing. Part of the works supports the conclusion with the results of the histological study, according to which the use of autologous plasma contributed to the early appearance of granulation, accelerating epithelialization and stimulating angiogenesis process in wounds [12,17].
Thus, among the published studies, some of which included extensive sampling frame, the results were often contradictory. Nevertheless, most studies have established that PRP had a significantly positive impact on the rate of surgical and acute wounds healing, transplanted flap survival indicators of flaps during reconstructive operations [17, 20].
With the increase of our understanding of platelet-rich plasma action on the healing of acute wounds, the usage of autologous plasma can improve the healing of soft tissue at surgical patients. If the application of platelet rich plasma accelerates healing of acute wounds of the soft tissues, it can prevent and reduce some postoperative complications, especially, in the case, where the complications caused by slow regeneration process [12].
Table 1 - Results of the use of PRP in different animal and human studies
|
Results of controlled animal studies |
||||
|
1 |
2 |
3 |
4 |
5 |
|
Author |
Year |
Studyprotocol |
Positiveeffect |
Lackofeffect |
|
Hanet al. |
2007 |
Number of subjects - 9 mice with diabetes. Application of platelet-rich plasma on the 5 mm punch wounds. |
The essential difference between two groups: a quick and complete healing (epithelialization of the punched skin in mice with diabetes) occurred in the experimental group on day 10. |
|
|
Leeet al. |
2008 |
Number of subjects - 15 rabbits.Four full thickness wounds (2.5 x 2.5 cm.) on the back of rabbits. The fourth wound was served as a control. Application of PRP on wounds. Histomorphological study. |
Use of PRP enhances wound healing by reducing the contraction rate with a tendency to accelerate the migration of epithelial and angiogenic response. |
No difference regarding the healing rate in experimental and control wounds. |
|
Molina- |
2009 |
Number of subjects - 20 rabbits. |
The essential difference in |
|
I 148 I
|
Minano et al. |
Application of platelet-rich plasma on 6 mm punch wounds |
epithelialization of experimental wounds on day 7 |
||
|
OmidOstva retal. |
2015 |
Number of subjects - 30 rabbits. The 3 cm. skin defect. PRP was applied on the wound. Histological examination on 7, 14 and 21 days. |
In the experimental group wounds were smaller on 7, 14, 21 days than in controls. Histological decrease in wound size and increase vascularization were observed in the experimental group on 14 and especially on 21 days. |
|
|
Cho-HeeJee et al. |
2016 |
Number of subjects - 3 dogs. Each dog had 8 punch wounds: the treatment was performed by injection of PRP into the wound on the 2nd and 4th day; 4 control wounds were treated with saline. Macro and microscopic examination on 7 and 14 days. |
An accelerated re-epithelialization and epithelial differentiation in the experimental wounds.PRP treated wounds showed more granulation formation and angiogenesis on day 7, more granulation formation and collagen deposition were observed on day 14 than in control wound. |
|
|
Results of controlled human studies |
||||
|
David B.Hom et al. |
2007 |
Number of patients - 8. Five full-thickness skin punch wounds (4 mm diameter) was conducted on the thighs. PRP was applied topically on the wounds on the day of surgery and on the 7th day. An antibiotic ointment and a semiocclusive dressing was applied on the other thigh. Studying results on day 1, 7, 10, 14, 17, 21, 24, 28, 31, 35, 42. |
The study confirmed the acceleration of wound healing time. The complete epithelialization of experimental wounds on day 7, the early appearance of granulation in comparison with control wounds. |
|
|
John Yoo et al. |
2008 |
52 patients (26 - experimental group, 26 - control group). Hemithyroidectomy was used as a model for the study because of its consistent surgical technique. Autologous PRP and PPP were applied during wound closure in the treatment group, while saline was applied in the controls. PRP treatment was sprayed onto the wound bed. |
Significant differences between two groups in the amount of cumulative drainage in the first 24 hours. Conclusion of the study - autologous plasma can be used as an alternative to commercial fibrin glues. |
There were no significant differences in the assessment of the level of pain in postoperative period in two groups |
|
Khalafi et al. |
2008 |
Number of patients - 1128. A patient group receiving topical application of platelet rich and platelet poor plasma during closure of their chest and leg surgical incisions. |
Significant difference for the test group: decreasing of the chest infection |
Other differences in the rate of healing of surgical wounds in the sternal region and in the saphenous vein harvest site were not found. |
|
Kazakos et al. |
2008 |
Number of patients - 59. Application of the platelet rich gel once per week on acute limb soft tissue wounds. |
Significant difference in wound healing time: 21.26 days in the experimental group versus 40.6 in the control group. |
|
|
Danielsen P. et al. |
2008 |
Number of patients - 20. Application of autologous platelet-rich fibrin on the donor sites and meshed split-thickness skin autografts area. |
Significant differences in the epithelialization were not found |
|
|
MichailSpyr idakis et al. |
2009 |
Number of patients - 52. Use of platelet-rich plasma twice a day on 4 and 12 days after excision of pilonidal sinus. |
A significant difference in the healing of surgical wounds. Patients reported about pain reduction. Reduction of recovery time and improvement the quality of life were observed. |
|
|
C.Eichler et al. |
2015 |
Number of patients - 120. Injection of the platelet-rich plasma was administered to wounds after surgical procedure for port removal. During questionnaire pain, mobility, sleep discomfort, satisfaction with postoperative results were evaluated. |
The final results showed that the pain in arm, mobility, discomfort during sleep, quality of life were not significantly different between control and experimental groups. |
|
|
Results of uncontrolled human studies |
||||
|
Kakudo et al. |
2011 |
Number of patients - 1 patient. Comparison of untreated and treated with platelet-rich plasma splitthickness skin graft donor sites. |
Acceleration of epithelialization in experimental group was observed. Pain during dressing was less pronounced. On the 13th day a skin biopsy showed much pronounced thickness of the |
|
|
epidermis and the number of newly formed blood vessels in the dermis. |
||||
|
Vincenzo Iervolino et al. |
2013 |
Number of patients - 10. Application of platelet rich plasma once per week on cutaneous radiation dermatitis after excision of sarcoma and radiotherapy. |
The patients had good compliance levels, fewer doctor visits. Good results in treatment of poorly healing surgical wounds, caused by the effect of radiation therapy. |
|
|
Vaclav Prochazka et al. |
2014 |
Number of patients - 18. After graft transplantation postoperative wound coated with platelet-rich plasma. Evaluation of the graft survival. Histological examination. Laser Doppler imaging at first two weeks and after 1, 3, 6, 12 months. |
The healing of postoperative wounds and healing of the flap accompanied by fewer complications. Decrease the number of rejections. The use of PRP led to physiological revascularization in 1-3 months. In postoperative period there was a decrease in pain and a reduction in the dose of analgesics taken by patients. |
REFERENCES
Conclusion:
In most studies authors noted effectiveness of platelet rich plasma in acceleration of acute wound healing[8 - 17]. Some of them shows interesting observation on reducing complications [17, 21]. All studies anyway shows that the acceleration of wound healing caused by action of growth factors contained in platelets of plasma.
Areas of misunderstanding and misbelieves: within one study authors show the efficacy of platelet rich plasma in reducing complications - wound infection, but no effect on the rate of healing [21]. The number of research subjects in some studies was large, in others was small (although the study was controlled). That's why it was difficult to compare the results of these studies. In different studies authors use different protocols to obtain platelet-rich plasma, there is no standard protocol. Different countries use different methods. Some authors use the plasma in the form of applications, others irrigate wound with platelet rich plasms before suturing or inject it directly to the wounds.
- Hall MP, Band PA, Meislin RT, Jazrawi LM, Cardone DA. Platelet-rich plasma: current concepts and application in sports medicine // Journal of the American Academy of Orthopaedic Surgeons. - 2009. - №10. - Р. 602-608.
- Singh R, Rohilla R, Dhayal R, Sen R, Sehgal P. Role of local application of autologous platelet-rich plasma in the management of pressure ulcers in spinal cord injury patients // Spinal Cord [serial online]. - 2014. - №52(11). - Р. 809-816.
- Heffner J, Holmes J, Dorion H, et al. Bone marrow-derived mesenchymal stromal cells and platelet-rich plasma on a collagen matrix to improve fascial healing // Hernia: The Journal Of Hernias And Abdominal Wall Surgery. - 2012. - №16(6). - Р. 677-687.
- Klaassen M, Pietrzak W. Platelet-rich plasma application and heterotopic bone formation following total hip arthroplasty // Journal Of Investigative Surgery: The Official Journal Of The Academy Of Surgical Research. - 2011. - №24(6). - Р. 257-261.
- Lyras D, Kazakos K, Patsouris E, et al. Immunohistochemical study of angiogenesis after local administration of platelet-rich plasma in a patellar tendon defect // International Orthopaedics. - 2010. - №34(1). - Р. 143-148.
- Vogrin M, Rupreht M, Rozman P, et al. Effects of a platelet gel on early graft revascularization after anterior cruciate ligament reconstruction: a prospective, randomized, double-blind, clinical trial. European Surgical Research // Europaische Chirurgische Forschung. - 2010. - №45(2). - Р. 77-85.
- Motolese A, Vignati F, Antelmi A, Saturni V. Effectiveness of platelet-rich plasma in healing necrobiosis lipoidicadiabeticorum ulcers // Clinical And Experimental Dermatology. - 2015. - №40(1). - Р. 39-41.
- Han SK, Kim DW, Jeong SH, Hong YT, Woo HS, Kim WK, et al. Potential use of blood bank platelet concentrates to accelerate wound healing of diabetic ulcers // Ann PlastSurg. - 2007. - №59. - Р. 532-537.
- Molina-Minano F, Lopez-Jornet P, Camacho-Alonso F, Vicente-Ortega V. The use of plasma rich in growth factors on wound healing in the skin: experimental study in rabbits // Int Wound J. - 2009. - №6. - Р. 145-148.
- Omid Ostvar, Sahar Shadvar, EmadYahaghi, Kamran Azma, Amir FarshidFayyaz, Koorosh Ahmadi and IradjNowrouzian. Effect of plateletrich plasma on the healing of cutaneous defects exposed to acute to chronic wounds: a clinico-histopathologic study on rabbits // Diagnostic Pathology. - 2015. - №10. - Р. 85-91.
- Cho-HeeJee, Na-Young Eom, Hyo-Mi Jang, Hae-Won Jung, Eul-Soo Choi, Jin-Hee Won, Il-Hwa Hong, Byeong-Teck Kang, Dong WookJeong, Dong-In Jung. Effect of autologous platelet-rich plasma application on cutaneous wound healing in dogs // J Vet Sci. - 2016. - №17(1). - Р. 79 - 87.
- Hom DB, Linzie BM, Huang TC. The healing effects of autologous platelet gel on acute human skin wounds // Arch Facial PlastSurg. - 2007. - №9. - Р. 174-183.
- Kazakos K, Lyras DN, Verettas D, Tilkeridis K, Tryfonidis M. The use of autologous PRP gel as an aid in the management of acute trauma wounds // Injury. - 2009. - №40. - Р. 801-805.
- Spyridakis M, Christodoulidis G, Chatzitheofilou C, Symeonidis D, Tepetes K. The role of the platelet-rich plasma in accelerating the wound-healing process and recovery in patients being operated for pilonidal sinus disease: preliminary results // World J Surg. - 2009. - №33. - Р. 1764-1769.
- Kakudo N, Kushida S, Minakata T, Suzuki K, Kusumoto K. Platelet-rich plasma promotes epithelialization and angiogenesis in a splitthickness skin graft donor site // Med MolMorphol. - 2011. - №44(4). - Р. 233-236.
- Vincenzo Iervolino, Gaetano Di Costanzo, Rosa Azzaro, Anna Maria Diodatoet all. Platelet gel in cutaneous radiation dermatitis // Support Care Cancer. - 2013. - №21. - Р. 287-293.
- Vaclav Prochazka, Hana Klosova, Jiri Stetinsky, JaromirGumulec, Katerina Vitkovad, Dana Salounovae. Addition of platelet concentrate to Dermo-Epidermal Skin Graft in deep burn trauma reduces scarring and need for revision surgeries // Biomed Pap Med FacUnivPalacky Olomouc Czech Repub. - 2014. - №158(2). - Р. 242-258.
- Lee HW, Reddy MS, Geurs N, Palcanis KG, Lemons JE, Rahemtulla FG, et al. Efficacy of platelet-rich plasma on wound healing in rabbits // J Periodontol. - 2008. - №79. - Р. 691-696.
- Khalafi RS, Bradford DW, Wilson MG. Topical application of autologous blood products during surgical closure following a coronary artery bypass graft // Eur J CardiothoracSurg. - 2008. - №34. - Р. 360-364.
- Danielsen P, Jorgensen B, Karlsmark T, Jorgensen LN, Agren MS. Effect of topical autologous platelet-rich fibrin versus no intervention on epithelialization of donor sites and meshed split-thickness skin autografts: a randomized clinical trial // PlastReconstrSurg. - 2008. - №122. - Р. 1431-1440.
- John Yoo, Kathryn Roth, Brian Hughes, Kevin Fung, Jason Franklin, Howard Lampe, William S. Pietrzak. Evaluation of postoperative drainage with applicatio n of platelet-rich and platelet-poor plasma following hemithyroidectomy: a randomized controlled clinical trial // Head & neck. - 2008. - №10. - Р. 1552 - 1558.
- Eichler C, Najafpour M, Sauerwald A, Puppe J, Warm M. Platelet-Rich Plasma in the Treatment of Subcutaneous Venous Access Device Scars: A Head-to-Head Patient Survey // BioMedResearchInternational. - 2015. - Vol. 2. - Р. 630-639.